US10610167B2 - Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing - Google Patents
Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathingDownload PDFInfo
- Publication number
- US10610167B2 US10610167B2US13/967,517US201313967517AUS10610167B2US 10610167 B2US10610167 B2US 10610167B2US 201313967517 AUS201313967517 AUS 201313967517AUS 10610167 B2US10610167 B2US 10610167B2
- Authority
- US
- United States
- Prior art keywords
- sdb
- patient
- related information
- display device
- processors
- Prior art date
- Legal status (The legal status is an assumption and is not a legal conclusion. Google has not performed a legal analysis and makes no representation as to the accuracy of the status listed.)
- Expired - Fee Related, expires
Links
- 230000029058respiratory gaseous exchangeEffects0.000titleclaimsabstractdescription39
- 238000012544monitoring processMethods0.000titleclaimsdescription18
- 230000002526effect on cardiovascular systemEffects0.000titleabstractdescription36
- 238000000034methodMethods0.000titledescription18
- 238000004891communicationMethods0.000claimsabstractdescription8
- 230000004044responseEffects0.000claimsabstractdescription8
- 208000008784apneaDiseases0.000claimsdescription16
- 206010021079HypopnoeaDiseases0.000claimsdescription14
- 238000009423ventilationMethods0.000claimsdescription10
- 206010041235SnoringDiseases0.000claimsdescription9
- 208000003417Central Sleep ApneaDiseases0.000claimsdescription7
- QVGXLLKOCUKJST-UHFFFAOYSA-Natomic oxygenChemical compound[O]QVGXLLKOCUKJST-UHFFFAOYSA-N0.000claimsdescription5
- 230000000414obstructive effectEffects0.000claimsdescription5
- 229910052760oxygenInorganic materials0.000claimsdescription5
- 239000001301oxygenSubstances0.000claimsdescription5
- 206010041349SomnolenceDiseases0.000claimsdescription4
- 208000032140SleepinessDiseases0.000claimsdescription3
- 230000037321sleepinessEffects0.000claimsdescription3
- 208000000059DyspneaDiseases0.000claims1
- 206010013975DyspnoeasDiseases0.000claims1
- 238000002644respiratory therapyMethods0.000claims1
- 201000002859sleep apneaDiseases0.000description37
- 208000037998chronic venous diseaseDiseases0.000description14
- 206010019280Heart failuresDiseases0.000description11
- 208000001797obstructive sleep apneaDiseases0.000description11
- 208000024172Cardiovascular diseaseDiseases0.000description10
- 230000000747cardiac effectEffects0.000description10
- 230000036772blood pressureEffects0.000description9
- 201000010099diseaseDiseases0.000description9
- 208000037265diseases, disorders, signs and symptomsDiseases0.000description9
- 206010020772HypertensionDiseases0.000description8
- 239000008280bloodSubstances0.000description7
- 210000004369bloodAnatomy0.000description7
- 238000003745diagnosisMethods0.000description7
- 230000037361pathwayEffects0.000description7
- 230000000241respiratory effectEffects0.000description6
- 208000006011StrokeDiseases0.000description5
- 238000005229chemical vapour depositionMethods0.000description5
- 101800000407Brain natriuretic peptide 32Proteins0.000description4
- 206010007559Cardiac failure congestiveDiseases0.000description4
- 230000008901benefitEffects0.000description4
- 239000007789gasSubstances0.000description4
- 230000002093peripheral effectEffects0.000description4
- 230000001225therapeutic effectEffects0.000description4
- 206010003119arrhythmiaDiseases0.000description3
- 230000006793arrhythmiaEffects0.000description3
- 230000003434inspiratory effectEffects0.000description3
- 208000010125myocardial infarctionDiseases0.000description3
- 238000002496oximetryMethods0.000description3
- 238000004018waxingMethods0.000description3
- CURLTUGMZLYLDI-UHFFFAOYSA-NCarbon dioxideChemical compoundO=C=OCURLTUGMZLYLDI-UHFFFAOYSA-N0.000description2
- 208000031229CardiomyopathiesDiseases0.000description2
- 150000003943catecholaminesChemical class0.000description2
- 230000008859changeEffects0.000description2
- 208000029078coronary artery diseaseDiseases0.000description2
- 238000001514detection methodMethods0.000description2
- 206010012601diabetes mellitusDiseases0.000description2
- 230000007774longtermEffects0.000description2
- 238000007726management methodMethods0.000description2
- 230000002644neurohormonal effectEffects0.000description2
- 238000001441oximetry spectrumMethods0.000description2
- 230000002861ventricularEffects0.000description2
- 208000018262Peripheral vascular diseaseDiseases0.000description1
- 208000032109Transient ischaemic attackDiseases0.000description1
- 230000001154acute effectEffects0.000description1
- 230000003044adaptive effectEffects0.000description1
- 230000009118appropriate responseEffects0.000description1
- 230000037007arousalEffects0.000description1
- 208000006673asthmaDiseases0.000description1
- 230000010455autoregulationEffects0.000description1
- 230000009286beneficial effectEffects0.000description1
- 230000005540biological transmissionEffects0.000description1
- 210000004204blood vesselAnatomy0.000description1
- 229910002092carbon dioxideInorganic materials0.000description1
- 239000001569carbon dioxideSubstances0.000description1
- 230000001269cardiogenic effectEffects0.000description1
- 208000026106cerebrovascular diseaseDiseases0.000description1
- 238000013479data entryMethods0.000description1
- 238000013500data storageMethods0.000description1
- 230000003247decreasing effectEffects0.000description1
- 230000002542deteriorative effectEffects0.000description1
- 229940079593drugDrugs0.000description1
- 239000003814drugSubstances0.000description1
- 238000013399early diagnosisMethods0.000description1
- 230000000694effectsEffects0.000description1
- 238000011156evaluationMethods0.000description1
- 238000001914filtrationMethods0.000description1
- 239000012634fragmentSubstances0.000description1
- 230000001631hypertensive effectEffects0.000description1
- 238000005259measurementMethods0.000description1
- 238000012986modificationMethods0.000description1
- 230000004048modificationEffects0.000description1
- 239000002243precursorSubstances0.000description1
- 230000036316preloadEffects0.000description1
- 230000008569processEffects0.000description1
- 238000011084recoveryMethods0.000description1
- 208000023504respiratory system diseaseDiseases0.000description1
- 238000012552reviewMethods0.000description1
- 230000033764rhythmic processEffects0.000description1
- 238000012216screeningMethods0.000description1
- 230000006641stabilisationEffects0.000description1
- 238000011105stabilizationMethods0.000description1
- 208000024891symptomDiseases0.000description1
- 238000002560therapeutic procedureMethods0.000description1
- 238000013022ventingMethods0.000description1
Images
Classifications
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B5/00—Measuring for diagnostic purposes; Identification of persons
- A61B5/72—Signal processing specially adapted for physiological signals or for diagnostic purposes
- A61B5/7271—Specific aspects of physiological measurement analysis
- A61B5/7282—Event detection, e.g. detecting unique waveforms indicative of a medical condition
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B5/00—Measuring for diagnostic purposes; Identification of persons
- A61B5/02—Detecting, measuring or recording for evaluating the cardiovascular system, e.g. pulse, heart rate, blood pressure or blood flow
- A61B5/0205—Simultaneously evaluating both cardiovascular conditions and different types of body conditions, e.g. heart and respiratory condition
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B5/00—Measuring for diagnostic purposes; Identification of persons
- A61B5/48—Other medical applications
- A61B5/4806—Sleep evaluation
- A61B5/4818—Sleep apnoea
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B5/00—Measuring for diagnostic purposes; Identification of persons
- A61B5/74—Details of notification to user or communication with user or patient; User input means
- A61B5/742—Details of notification to user or communication with user or patient; User input means using visual displays
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61B—DIAGNOSIS; SURGERY; IDENTIFICATION
- A61B5/00—Measuring for diagnostic purposes; Identification of persons
- A61B5/74—Details of notification to user or communication with user or patient; User input means
- A61B5/7475—User input or interface means, e.g. keyboard, pointing device, joystick
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/0051—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes with alarm devices
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/0057—Pumps therefor
- A61M16/0066—Blowers or centrifugal pumps
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/0057—Pumps therefor
- A61M16/0066—Blowers or centrifugal pumps
- A61M16/0069—Blowers or centrifugal pumps the speed thereof being controlled by respiratory parameters, e.g. by inhalation
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/021—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes operated by electrical means
- A61M16/022—Control means therefor
- A61M16/024—Control means therefor including calculation means, e.g. using a processor
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/06—Respiratory or anaesthetic masks
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/08—Bellows; Connecting tubes ; Water traps; Patient circuits
- A61M16/0816—Joints or connectors
- A61M16/0841—Joints or connectors for sampling
- A61M16/085—Gas sampling
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/08—Bellows; Connecting tubes ; Water traps; Patient circuits
- A61M16/0875—Connecting tubes
- G06F19/3418—
- G—PHYSICS
- G16—INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR SPECIFIC APPLICATION FIELDS
- G16H—HEALTHCARE INFORMATICS, i.e. INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR THE HANDLING OR PROCESSING OF MEDICAL OR HEALTHCARE DATA
- G16H10/00—ICT specially adapted for the handling or processing of patient-related medical or healthcare data
- G16H10/20—ICT specially adapted for the handling or processing of patient-related medical or healthcare data for electronic clinical trials or questionnaires
- G—PHYSICS
- G16—INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR SPECIFIC APPLICATION FIELDS
- G16H—HEALTHCARE INFORMATICS, i.e. INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR THE HANDLING OR PROCESSING OF MEDICAL OR HEALTHCARE DATA
- G16H40/00—ICT specially adapted for the management or administration of healthcare resources or facilities; ICT specially adapted for the management or operation of medical equipment or devices
- G16H40/60—ICT specially adapted for the management or administration of healthcare resources or facilities; ICT specially adapted for the management or operation of medical equipment or devices for the operation of medical equipment or devices
- G16H40/63—ICT specially adapted for the management or administration of healthcare resources or facilities; ICT specially adapted for the management or operation of medical equipment or devices for the operation of medical equipment or devices for local operation
- G—PHYSICS
- G16—INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR SPECIFIC APPLICATION FIELDS
- G16H—HEALTHCARE INFORMATICS, i.e. INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR THE HANDLING OR PROCESSING OF MEDICAL OR HEALTHCARE DATA
- G16H50/00—ICT specially adapted for medical diagnosis, medical simulation or medical data mining; ICT specially adapted for detecting, monitoring or modelling epidemics or pandemics
- G16H50/30—ICT specially adapted for medical diagnosis, medical simulation or medical data mining; ICT specially adapted for detecting, monitoring or modelling epidemics or pandemics for calculating health indices; for individual health risk assessment
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M16/00—Devices for influencing the respiratory system of patients by gas treatment, e.g. ventilators; Tracheal tubes
- A61M16/0003—Accessories therefor, e.g. sensors, vibrators, negative pressure
- A61M2016/003—Accessories therefor, e.g. sensors, vibrators, negative pressure with a flowmeter
- A61M2016/0033—Accessories therefor, e.g. sensors, vibrators, negative pressure with a flowmeter electrical
- A61M2016/0039—Accessories therefor, e.g. sensors, vibrators, negative pressure with a flowmeter electrical in the inspiratory circuit
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M2205/00—General characteristics of the apparatus
- A61M2205/35—Communication
- A61M2205/3546—Range
- A61M2205/3569—Range sublocal, e.g. between console and disposable
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M2205/00—General characteristics of the apparatus
- A61M2205/35—Communication
- A61M2205/3576—Communication with non implanted data transmission devices, e.g. using external transmitter or receiver
- A61M2205/3592—Communication with non implanted data transmission devices, e.g. using external transmitter or receiver using telemetric means, e.g. radio or optical transmission
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61M—DEVICES FOR INTRODUCING MEDIA INTO, OR ONTO, THE BODY; DEVICES FOR TRANSDUCING BODY MEDIA OR FOR TAKING MEDIA FROM THE BODY; DEVICES FOR PRODUCING OR ENDING SLEEP OR STUPOR
- A61M2230/00—Measuring parameters of the user
- A61M2230/04—Heartbeat characteristics, e.g. ECG, blood pressure modulation
- G—PHYSICS
- G16—INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR SPECIFIC APPLICATION FIELDS
- G16H—HEALTHCARE INFORMATICS, i.e. INFORMATION AND COMMUNICATION TECHNOLOGY [ICT] SPECIALLY ADAPTED FOR THE HANDLING OR PROCESSING OF MEDICAL OR HEALTHCARE DATA
- G16H10/00—ICT specially adapted for the handling or processing of patient-related medical or healthcare data
- G16H10/60—ICT specially adapted for the handling or processing of patient-related medical or healthcare data for patient-specific data, e.g. for electronic patient records
Definitions
- This inventionrelates to methods and apparatus for treating and monitoring sleep disordered breathing (“SDB”) in patients with cardiovascular disease or otherwise monitoring the cardiovascular condition of SDB patients.
- SDBsleep disordered breathing
- “Sleep-disordered breathing”generally refers to types of breathing disruption that occur during sleep.
- the most common form of sleep disordered breathingis obstructive sleep apnea (“OSA”).
- OSAobstructive sleep apnea
- OSAaffects approximately 20 million Americans—as many as asthma or diabetes. Less than 10% of people with OSA have been diagnosed and fewer have been treated. Loud, intermittent snoring, apneas, and hypopneas characterize OSA. Because the symptoms of sleep apnea present themselves as a result of a precursor, SDB has become the general term used to describe any disease state that manifests apneas and/or hypopneas during sleep. Apneas and hypopneas interfere with gas exchange, fragment sleep, and frequently cause oxygen desaturations. In severe cases, patients may experience these oxygen desaturations and arousals from sleep hundreds of times each night.
- CPAP treatmentacts as a pneumatic splint of the airway by the provision of a positive pressure, usually in the range 4-20 cm H 2 O.
- the airis supplied to the airway by a motor driven blower that is coupled via an air delivery hose to a nose (or nose and/or mouth) mask sealed with the patient's face.
- CPAP treatmentmay be provided by bi-level ventilators, proportional assist ventilators and servo-controlled ventilators. Such devices are typically used by the patient on a daily basis before and during sleep.
- nasal CPAP treatment of OSAmay involve the use of an automated blower, such as the AUTOSET TTM device or AUTOSET SPIRITTM available from ResMed Ltd.
- suitable nasal CPAP masksare the MIRAGETM nasal mask and the MIRAGETM full face mask also available from ResMed Ltd.
- the AUTOSET TTM devicecontinuously monitors the state of the patient's airway and determines an appropriate pressure to treat the patient, increasing it or decreasing it as necessary.
- bi-level pressuresare delivered to the patient as in the VPAP IITM devices also available from ResMed Ltd.
- CVDcardiovascular disease
- CVDsare diseases that have an impact on the correct functioning of the heart and blood vessels.
- strokecerebrovascular diseases
- other significant CVDsinclude myocardial infarction (heart attack), congestive heart failure (“CHF”), transient ischaemic attacks (“TIA”) and peripheral vascular diseases, to name a few.
- CHFcongestive heart failure
- TIAtransient ischaemic attacks
- peripheral vascular diseasesto name a few.
- CPAP deviceshave in the past been used for the treatment of SDB in CVD patients.
- a form of pressure treatmenthas been directed at treatment of cardiac failure and Cheyne-Stokes breathing.
- AUTOSET CSTMalso provided by ResMed Ltd.
- pressure supportis varied in phase with patient respiration in such a manner to oppose the waxing and waning changes in patient respiration that characterize Cheyne-Stokes breathing.
- the deviceis the subject of U.S. Pat. No. 6,532,959, the entire disclosure of which is incorporated herein by reference.
- CPAP treatmenthas also been recognized as a beneficial treatment of stroke.
- the use of CPAPtreats stroke patients by improving arterial blood oxygen levels and reducing arterial carbon dioxide levels as well as improving auto-regulation of, for example, blood pressure, cardiac output and ventilation. Improvements in morbidity, such as rate and degree of recovery of vital signs and patient stabilization in the acute phase, is an expected benefit.
- U.S. Pat. No. 5,794,615teaches a system including methods and apparatus for treatment of congestive heart failure.
- the systeminvolves applying separate and independent gains to flow rates of pressurized gas delivered to a patient during inspiratory and expiratory phases of a respiratory cycle.
- the pressure supportis disclosed as reducing cardiac pre-load and after load.
- apparatuscomprising a sleep disordered breathing treatment unit and a unit for monitoring the patient for indications of cardiovascular disease.
- the inventionprovides methods and apparatus useful for cardiovascular disease patients or potential cardiovascular disease patients with sleep disordered breathing.
- the deviceis capable of delivering positive airway pressure at therapeutic levels for treatment of sleep disordered breathing.
- the devicecan be configured with one or more protocols that may be utilized in the provision of such pressure treatment. Over the course of one or more sessions of such treatment, the device may be configured to detect and record events associated with sleep disordered breathing, such as apnea, hypopneas, partial obstruction, snoring, pressure versus time, flow versus time, and leak for future analysis.
- the deviceis configured to detect or prompt and accept as input additional information concerning the cardiovascular condition of the patient including, for example, blood pressure, heart rate, oximetry data, electrocardiogram data, Holter Analysis results (including arrhythmia and heart-rate variability summaries), body mass index (including height and weight data), Left Ventricular Ejection Fraction (“LVEF”), six-minute walk data, B-type natriuretic peptide (“BNP”), cardiac output data, VO 2 max data, New York Heart Association Class (“NYHA”), ACC/AHA Heart Failure Stage, Quality of Life data (including, for example, Epworth Sleepiness Scale, Berlin Questionnaire, Minnesota Living with Heart Failure Questionnaire, and Kansas City Cardiomyopathy Questionnaire), peripheral arterial tone (“PAT”), and Key neuro-hormonal levels (e.g., catecholamine levels).
- additional information concerning the cardiovascular condition of the patientincluding, for example, blood pressure, heart rate, oximetry data, electrocardiogram data, Holter Analysis results (including arrhythmia and heart-rate variability summaries), body mass index
- Such datamay be continuously or periodically recorded or entered into the device relative to time. With such data in the device associations may be observed or made between the cardiovascular information and sleep disordered breathing related events on a common time scale so that changes that occur approximately or substantially in common may be observed or tracked. Such data may be retrieved from or viewed on the device or accessed remotely by a physician or clinician for purposes of monitoring or diagnosis of the patient's SDB and/or a potential CVD.
- Another aspect of the inventionis a combination of products, services and business pathways for providing care of SDB and CVD co-morbid patients.
- FIG. 1shows an apparatus according to the invention.
- FIG. 2is a flow chart of a method for monitoring patient cardiovascular information.
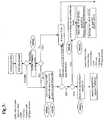
- FIGS. 3 & 4are flow charts showing business pathways in accordance with aspects of the invention.
- the inventioninvolves a pressure delivery device that may include a servo-controlled blower 2 , a mask 6 , and an air delivery conduit 8 for connection between the blower 2 and the mask 6 .
- Exhaust gasis vented via exhaust 13 .
- a flow sensor 4 f and/or pressure sensor 4 pmay also be utilized in which case mask flow may be measured using a pneumotachograph and differential pressure transducer or similar device to derive a flow signal F(t), and mask pressure is measured at a pressure tap using a pressure transducer to derive a pressure signal P mask (t).
- the pressure sensor 4 f and flow sensor 4 phave only been shown symbolically in FIG.
- Flow F(t) and pressure P mask (t)signals are sent to a controller or microprocessor 15 to derive a pressure request signal P request (t).
- a flow signal f(t) and pressure signal P mask (t)may be estimated or calculated in relation to the blower motor by monitoring current supplied to the motor and/or the speed of the motor as disclosed in U.S. Pat. Nos. 5,740,795, 6,332,463 or 6,237,593 without the provision of flow and pressure sensors as described above.
- the blower motor speedmay be held generally constant and pressure changes in the mask may be implemented by controlling an opening of a servo-valve that may variably divert/vent or deliver airflow to the mask.
- a controller 15 or processoris configured and adapted to implement the methodology described in more detail herein and may include integrated chips, a memory and/or other instruction or data storage medium.
- programmed instructions with the control methodologymay be coded on integrated chips in the memory of the device or such instructions may be loaded as software.
- the apparatuscan be used for many different pressure treatment therapies simply by adjusting the pressure delivery equation that is used to set the speed of the blower or to manipulate the venting with the release valve.
- the apparatuspreferably also includes a communication port or module 10 , for example, a wireless communication transceiver and/or a network card, for communication with other devices or computers such as hand-held display and control devices 12 .
- the apparatusmay further include additional interface 16 for connection to additional diagnosis or patient information gathering devices.
- a diagnosis unitmay optionally include a pulse oximeter 20 , respiratory movement sensors 22 such as a chest band, EEG & ECG 24 , EOG 25 and/or electrodes 28 for detecting cardiac rhythm.
- the oximetermay optionally be included in the main blower housing.
- an automated PCO 2 measurement device 21 or other non-invasive blood gas monitor/device for measuring PCO 2may be linked to provide an input data signal to the microprocessor 16 , for example, a device as taught in U.S. Pat. No. 5,630,413, the disclosure of which is incorporated by reference.
- Other automated measuring devicesmay also be included with the diagnosis unit as it relates to measuring other cardiovascular related information from the patient.
- the devicemay, for example, be configured to communicate/receive such information from its own display (e.g., LCD screen) and input device (e.g., keypad or buttons) or via telemetry or other communication link from a blood pressure monitor, heart rate monitor, oximetry monitor, ECG device, ECG Event Monitor, Holter monitor, automated tape measure, automated weight scale, treadmill device, blood analyzer device, cardiac output analyzer device, VO 2 max data device or peripheral arterial tone assessment device.
- a blood pressure monitore.g., LCD screen
- input devicee.g., keypad or buttons
- telemetry or other communication linkfrom a blood pressure monitor, heart rate monitor, oximetry monitor, ECG device, ECG Event Monitor, Holter monitor, automated tape measure, automated weight scale, treadmill device, blood analyzer device, cardiac output analyzer device, VO 2 max data device or peripheral arterial tone assessment device.
- a blood pressure monitore.g., heart rate monitor, oximetry monitor
- ECG deviceECG Event Monitor
- Holter monitor
- input and/or output devices 22may be included to display output signals and enter input signals for the microprocessor 16 .
- Various appropriate input and output devicessuch as keypads and display screens and other alternatives are known in the art.
- the apparatuscan interface with a variety of hand-held devices such as a Palm Pilot via wireless communication or it may interface with a network for transmission between the devices.
- a physicianmay, for example, remotely monitor, analyze or record the status or data history of a patient.
- remote devicesmay send to or retrieve from the apparatus any desired cardiovascular or other information.
- Such informationmay even be transmitted from the apparatus to a database of one or more patients.
- the treatment program that is being run on the patientcan be monitored and changed remotely. In the event patient data is transmitted over open networks, the data may be encrypted for purposes of patient confidentiality.
- the apparatusincorporates various pressure treatment protocols that may be used to treat the condition of the patient.
- the deviceprovides a generally constant pressure throughout a breathing cycle that may be therapeutic pressure or changes to such pressure set to treat SDB.
- the apparatusprovides a higher pressure to the mask during the inspiratory portion of the breathing cycle, a so-called IPAP (inspiratory positive airway pressure), and a lower pressure to the mask during the expiratory portion of the breathing cycle, a so-called EPAP (expiratory positive airway pressure).
- IPAPinspiratory positive airway pressure
- EPAPexpiratory positive airway pressure
- the treatment delivered by the apparatuscan smoothly vary in accordance with patient respiration to provide a smooth pressure waveform.
- the devicecalculates a continuous phase variable to provide support in phase with the patient's breathing cycle and calculates the pressure to be delivered in accordance with a pressure waveform template.
- the delivery of such pressureis disclosed in U.S. Pat. No. 6,532,957.
- pressuremay be supplied in proportion to patient respiratory airflow.
- pressure supportis varied in phase with patient respiration in such a manner to oppose the waxing and waning changes in patient respiration that characterize Cheyne-Stokes breathing.
- the methodology for such treatmentis disclosed in U.S. Pat. No. 6,532,959.
- the therapeutic pressure levels of the above protocolsmay be preset by a clinician or may be automatically adjusted or set by automatic detection of SDB related events, such as apneas (obstructive or central), hypopneas, partial obstruction, snoring, etc. as disclosed in U.S. Pat. No. 5,704,345 (Berthon-Jones).
- SDB related eventssuch as apneas (obstructive or central), hypopneas, partial obstruction, snoring, etc. as disclosed in U.S. Pat. No. 5,704,345 (Berthon-Jones).
- the IPAP or EPAP levelsmay be adjusted by the automated determination to hunt for a minimal pressure that will be required to prevent or alleviate obstruction.
- Other alternative methods to vary the therapeutic level of the pressure for treatment to a patient and to detect SDB eventsmay be utilized and are known in the art.
- leak airflowmay be determined by using a method such as taught in U.S. Pat. No. 6,152,129 (Berthon-Jones), the entire disclosure of which is incorporated herein by reference.
- Leak datamay also be recorded over time and stored in the device. Other known methods for determining leak may also be used by the device.
- the deviceprovides efficacy tracking by detecting and recording or scoring SDB events or related information or indices overtime, for example, by tracking or detecting central apneas, obstructive apneas, hypopneas, partial obstructions (e.g., flow flattening) or snoring. This is illustrated in step 44 of FIG. 2 .
- pressure and/or flow versus time datamay also be recorded for analysis.
- the devicepreferably performs compliance tracking in which the time on and time off of the mask are recorded with SDB related events for evaluation by statistical summaries and charting. Methods for detecting and recording such information are known in the art, and may be implemented as described in U.S. Pat. No. 5,704,345.
- the devicemay record AHI (apnea hypopnea index) over time or during particular time periods such as session-by-session, day-by-day, hour-by-hour, etc.
- AHIan AHI scoring scheme may be implemented as follows:
- the devicemay determine an index comparing central apneas versus obstructive apneas as disclosed in U.S. Pat. No. 6,832,609, the entire disclosure of which is incorporated by reference herein.
- a device of the inventionpreferably includes input devices for receiving or recording such based on the condition of the patient, continuously or periodically, so that preferably, as illustrated in step 46 of FIG. 2 , such information may be associated with changes in the sleep disordered breathing related information over time.
- Embodiments of the inventionmay include automated measuring apparatus that can generate signals associated with the automatically determined cardiovascular information for a processor of the device.
- the devicemay be pre-programmed to prompt or query for such information on a display or from another remote device, before use and/or periodically such as monthly, after three or six months, or some other timed period which may be based on use of the device (e.g., after 30 nights of use, etc.), so that such information may be measured or determined separately and input by a user on a keypad or other data entry device.
- queriesmay be pre-programmed into the device and appropriate responses can be input by the patient in response to prompting by the device.
- an apparatus of the inventionmay include automated blood pressure monitoring apparatus that may continuously or periodically monitor or measure blood pressure and record such information such as in an overnight summary versus time.
- the devicemay prompt for input of such information on a display and keypad without the provision of such an automated device.
- Such informationmay then be charted alone or in association with sleep disordered breathing related information or events, such as an AHI, on a comparable or similar time scale so that related changes may be observed or noted.
- the devicemay monitor and record heart rate and/or detailed echocardiogram data continuously or periodically.
- Such informationmay be detected by filtering cardiogenic flow from a respiratory flow signal as disclosed in U.S. Pat. No. 5,704,345 or by another available heart rate detector.
- heart rateBy recording such information over time, alone or on a similar time scale as sleep disordered breathing information, changes in heart rate may be observed or associated with changes in sleep disordered breathing to assist in tracking the condition of the patient.
- various embodiments of the devicemay optionally measure, prompt for and/or record/monitor additional cardiovascular information including oximetry data, blood sugar data, blood pressure data, electrocardiogram data, Holter Analysis results (including, e.g., arrhythmia, heart-rate and/or variability summaries), Body Mass Index, height and weight data, Left Ventricular Ejection Fraction (LVEF), Six-minute walk data, B-type natriuretic peptide (BNP), Cardiac Output data, VO 2 max data, New York Heart Association Class (NYHA), ACC/AHA Heart Failure Stage, Quality of Life data (including, e.g., Epworth Sleepiness Scale, Berlin Questionnaire, Minnesota Living with Heart Failure Questionnaire, and/or Kansas City Cardiomyopathy Questionnaire), Peripheral arterial tone (PAT) and Key neuro-hormonal levels (e.g., catecholamine levels).
- oximetry datablood sugar data
- blood pressure datablood pressure data
- electrocardiogram dataHolter Analysis results (including, e.g.,
- the devicemay be configured to monitor all of this information but the physician can preset the device to select one or more of the features for particular patients, which will then be monitored during their use.
- the deviceis pre-programmed with associated sets or groups of data selected from the cardiovascular information that are pertinent for specific cardiovascular patients. By selecting a particular patient type, the device can automatically be configured to monitor the pertinent cardiovascular information from the associated set or group of monitored data without monitoring unnecessary cardiovascular information for the particular patient.
- a hypertension patientmay be monitored for blood pressure, heart rate and Body Mass Index or a heart failure patient may be monitored for LVEF heart rate and cardiac output data, a diabetic may be monitored for blood sugar, etc.
- a hypertension patientmay be monitored for blood pressure, heart rate and Body Mass Index or a heart failure patient may be monitored for LVEF heart rate and cardiac output data, a diabetic may be monitored for blood sugar, etc.
- cardiovascular informationis preferably associated with the different types of cardiovascular patients.
- a physician or clinicianmay periodically access a substantial source of information for study or analysis, as illustrated by step 48 of FIG. 2 .
- the cardiovascular and SDB informationmay be periodically remotely transferred to the physician or it may be accessed directly through displays on the device. In this way, a physician may keep up with and observe the changing cardiovascular condition of the patient with minimal direct oversight or intervention.
- the devicecan be programmed with thresholds for comparison to the recorded cardiovascular information to trigger an alarm or send a message or generate a warning for the user, clinician or physician either directly on the device, or remotely, for example, over a secure electronic network to a database. For example, if the recorded or detected heart rate falls below an acceptable level, a warning or alarm may be generated. Similarly, if changes in weight, arrhythmia, blood pressure, blood sugar, heart variability, ECG data, etc. are recorded, automated warnings, alarms or messages may be generated by the device and manual or automated changes to the control of the device may be made such as a change in treatment protocol or a change to the set of monitored cardiovascular information such that additional cardiovascular information may be monitored.
- the devicemay switch from monitoring hypertension associated cardiovascular information to monitoring congestive heart failure associated cardiovascular information if changes in the hypertension related monitoring data suggest that the patient's cardiovascular condition is deteriorating.
- the device's treatment protocolmay switch from a standard bi-level protocol to one that delivers servo-controlled pressure changes intended to reduce waxing and waning changes associated with Cheyne-Stokes breathing.
- monitoring patientsis an important aspect of management of cardiovascular disease.
- nasal CPAP devicesalmost every night for the rest of the patient's life
- cardiovascular related treatment or diagnostic devicesmay be implemented to query for or measure SDB related information for the purpose of detecting SDB or otherwise determining a relationship between the cardiovascular condition of the patient and SDB.
- a Holter Monitor or cardiac event monitormay be configured or programmed to prompt a patient with an SDB questionnaire.
- the devicemay prompt a user with such questions as:
- the devicemay record, transmit or generate a warning to the user or physician to consider referral to a clinician or other physician for the purpose of undertaking a sleep diagnostic study to access the potential for SDB.
- a more detailed assessment of SDB related informationmay be implemented by the device. For example, it may prompt for the following:
- Gender(Male or Female)
- the number of positive responsesmay be tallied by the device to generate a SDB index which may be reported to a physician with a warning or other message.
- the SDB indexmay be compared to one or more thresholds and the degree of the need for a follow-up SDB study may be contained in a message or warning to the physician or user. For example, if the tally is 1 or 0, the message may identify that there is a low likelihood that the patient has an SDB condition or would need to follow-up with a sleep study. A higher tally, such as a 4 or higher, may result in a more significant or urgent warning message suggesting that there is a high or higher likelihood of SDB or a need for a full SDB assessment.
- Such datamay be combined with other sleep disordered breathing data recorded by the device, for example, an AHI, if the device is configured to record such data and may be included in the message or warning to the physician or user.
- cardiovascular related treatment or diagnostic devicemay be configured or programmed to make an assessment for SDB related information of the patient, for example, a blood pressure monitor, heart rate monitor, oximetry monitor, Holter Monitor or other ECG device or cardiac event monitor, automated tape measure, automated scale device for weight, treadmill device, blood analyzer device, cardiac output analyzer device, VO 2 max data device, peripheral arterial tone device etc.
- FIGS. 3 & 4show business pathways in accordance with the invention. Such pathways can be adopted by organisations caring for SBD and CVD co-morbid patients using the equipment shown in FIG. 1 .
- the pathwaysidentify steps to be taken, and identifies the appropriate re-imbursement codes.
- the pathwayscan be programmed into portable computers, such as PALM PILOT handheld computers, providing the practitioner with a ready reference for the appropriate codes, as well as allowing a highly skilled medical practitioner (such as a cardiologist) to delegate responsibility to their staff.
- a cardiology patientis given a questionnaire programmed into a handheld computer as discussed above.
- a positive result from the questionnaireprompts the device to suggest an unattended sleep study, for example with a Holter monitor, as well as reimbursement codes 95806 and 93230.
- the resultsare entered into the computer.
- a high AHI from the sleep studyindicates the potential presence of Obstructive Sleep Apnea (OSA) or Central Sleep Apnea (CSA).
- OSAObstructive Sleep Apnea
- CSACentral Sleep Apnea
- Patients with OSAmay be treated with an Automatic Positive Airway Pressure (APAP) device such as ResMed's AUTOSET SPIRIT.
- APAPAutomatic Positive Airway Pressure
- patients with CSAmay be treated with ResMed's VPAP III ST/A device, or Adaptive Servo Ventilation, such as provided by ResMed's AutoSet CS2 device.
- the decision processincludes oximetry or OSA screening by a device such as ResMed's APNEA LINK.
Landscapes
- Health & Medical Sciences (AREA)
- Life Sciences & Earth Sciences (AREA)
- Engineering & Computer Science (AREA)
- Public Health (AREA)
- General Health & Medical Sciences (AREA)
- Biomedical Technology (AREA)
- Veterinary Medicine (AREA)
- Animal Behavior & Ethology (AREA)
- Heart & Thoracic Surgery (AREA)
- Pulmonology (AREA)
- Medical Informatics (AREA)
- Emergency Medicine (AREA)
- Anesthesiology (AREA)
- Hematology (AREA)
- Pathology (AREA)
- Molecular Biology (AREA)
- Surgery (AREA)
- Physics & Mathematics (AREA)
- Biophysics (AREA)
- Physiology (AREA)
- Cardiology (AREA)
- Primary Health Care (AREA)
- Epidemiology (AREA)
- Artificial Intelligence (AREA)
- Computer Vision & Pattern Recognition (AREA)
- Psychiatry (AREA)
- Signal Processing (AREA)
- Data Mining & Analysis (AREA)
- Databases & Information Systems (AREA)
- General Business, Economics & Management (AREA)
- Business, Economics & Management (AREA)
- Measurement Of The Respiration, Hearing Ability, Form, And Blood Characteristics Of Living Organisms (AREA)
Abstract
Description
- (i) An apnea is scored if a 2 second moving average ventilation drops below 25% of a recent average ventilation (time constant=100 s) for at least 10 consecutive seconds,
- (ii) An hypopnea is scored if the 8 second moving average drops below 50% but not more than 25% of the recent average ventilation for 10 consecutive seconds.
Claims (20)
Priority Applications (1)
| Application Number | Priority Date | Filing Date | Title |
|---|---|---|---|
| US13/967,517US10610167B2 (en) | 2004-03-31 | 2013-08-15 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
Applications Claiming Priority (5)
| Application Number | Priority Date | Filing Date | Title |
|---|---|---|---|
| US55784604P | 2004-03-31 | 2004-03-31 | |
| PCT/US2005/010663WO2005096737A2 (en) | 2004-03-31 | 2005-03-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
| US10/598,914US7878198B2 (en) | 2004-03-31 | 2005-03-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
| US12/982,536US8517014B2 (en) | 2004-03-31 | 2010-12-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
| US13/967,517US10610167B2 (en) | 2004-03-31 | 2013-08-15 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
Related Parent Applications (1)
| Application Number | Title | Priority Date | Filing Date |
|---|---|---|---|
| US12/982,536ContinuationUS8517014B2 (en) | 2004-03-31 | 2010-12-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
Publications (2)
| Publication Number | Publication Date |
|---|---|
| US20130331713A1 US20130331713A1 (en) | 2013-12-12 |
| US10610167B2true US10610167B2 (en) | 2020-04-07 |
Family
ID=38233605
Family Applications (3)
| Application Number | Title | Priority Date | Filing Date |
|---|---|---|---|
| US10/598,914Expired - Fee RelatedUS7878198B2 (en) | 2004-03-31 | 2005-03-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
| US12/982,536Expired - LifetimeUS8517014B2 (en) | 2004-03-31 | 2010-12-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
| US13/967,517Expired - Fee RelatedUS10610167B2 (en) | 2004-03-31 | 2013-08-15 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
Family Applications Before (2)
| Application Number | Title | Priority Date | Filing Date |
|---|---|---|---|
| US10/598,914Expired - Fee RelatedUS7878198B2 (en) | 2004-03-31 | 2005-03-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
| US12/982,536Expired - LifetimeUS8517014B2 (en) | 2004-03-31 | 2010-12-30 | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing |
Country Status (1)
| Country | Link |
|---|---|
| US (3) | US7878198B2 (en) |
Cited By (2)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US20230104018A1 (en)* | 2021-10-05 | 2023-04-06 | Ndustry-Academic Cooperation Foundation, Yonsei University | Cardiovascular disease risk analysis system and method considering sleep apnea factors |
| USD1014517S1 (en) | 2021-05-05 | 2024-02-13 | Fisher & Paykel Healthcare Limited | Display screen or portion thereof with graphical user interface |
Families Citing this family (90)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US12220530B2 (en)* | 2004-06-04 | 2025-02-11 | New York University | System and method for automated titration of continuous positive airway pressure using an obstruction index |
| EP1893264B1 (en)* | 2005-06-14 | 2016-02-24 | ResMed Limited | Acclimatization therapy for first time cpap and niv users |
| US7942824B1 (en) | 2005-11-04 | 2011-05-17 | Cleveland Medical Devices Inc. | Integrated sleep diagnostic and therapeutic system and method |
| US8545416B1 (en)* | 2005-11-04 | 2013-10-01 | Cleveland Medical Devices Inc. | Integrated diagnostic and therapeutic system and method for improving treatment of subject with complex and central sleep apnea |
| US8172766B1 (en)* | 2005-11-04 | 2012-05-08 | Cleveland Medical Devices Inc. | Integrated sleep diagnosis and treatment device and method |
| US20070129644A1 (en)* | 2005-12-02 | 2007-06-07 | Glenn Richards | Sleep disorder screening program |
| US8015972B2 (en)* | 2006-01-03 | 2011-09-13 | Shahzad Pirzada | System, device and process for remotely controlling a medical device |
| EP1978460B1 (en)* | 2007-04-05 | 2014-01-22 | ResMed R&D Germany GmbH | Monitoring device and method |
| US8369944B2 (en) | 2007-06-06 | 2013-02-05 | Zoll Medical Corporation | Wearable defibrillator with audio input/output |
| US8271082B2 (en) | 2007-06-07 | 2012-09-18 | Zoll Medical Corporation | Medical device configured to test for user responsiveness |
| US7974689B2 (en)* | 2007-06-13 | 2011-07-05 | Zoll Medical Corporation | Wearable medical treatment device with motion/position detection |
| US8140154B2 (en) | 2007-06-13 | 2012-03-20 | Zoll Medical Corporation | Wearable medical treatment device |
| US8838217B2 (en)* | 2009-11-10 | 2014-09-16 | Makor Issues And Rights Ltd. | System and apparatus for providing diagnosis and personalized abnormalities alerts and for providing adaptive responses in clinical trials |
| US8706215B2 (en) | 2010-05-18 | 2014-04-22 | Zoll Medical Corporation | Wearable ambulatory medical device with multiple sensing electrodes |
| US9008801B2 (en) | 2010-05-18 | 2015-04-14 | Zoll Medical Corporation | Wearable therapeutic device |
| US9937355B2 (en) | 2010-11-08 | 2018-04-10 | Zoll Medical Corporation | Remote medical device alarm |
| JP5963767B2 (en) | 2010-12-09 | 2016-08-03 | ゾール メディカル コーポレイションZOLL Medical Corporation | Electrode assembly |
| JP5988991B2 (en) | 2010-12-10 | 2016-09-07 | ゾール メディカル コーポレイションZOLL Medical Corporation | Wearable treatment device |
| US9427564B2 (en) | 2010-12-16 | 2016-08-30 | Zoll Medical Corporation | Water resistant wearable medical device |
| US20120157794A1 (en)* | 2010-12-20 | 2012-06-21 | Robert Goodwin | System and method for an airflow system |
| US9011346B2 (en) | 2011-01-27 | 2015-04-21 | The Board Of Trustees Of The Leland Stanford Junior University | Systems and methods for monitoring the circulatory system |
| WO2012135062A1 (en) | 2011-03-25 | 2012-10-04 | Zoll Medical Corporation | Selection of optimal channel for rate determination |
| WO2012135028A1 (en) | 2011-03-25 | 2012-10-04 | Zoll Medical Corporation | Method of detecting signal clipping in a wearable ambulatory medical device |
| US9135398B2 (en) | 2011-03-25 | 2015-09-15 | Zoll Medical Corporation | System and method for adapting alarms in a wearable medical device |
| US9684767B2 (en) | 2011-03-25 | 2017-06-20 | Zoll Medical Corporation | System and method for adapting alarms in a wearable medical device |
| JP2014516654A (en) | 2011-05-02 | 2014-07-17 | ゾール メディカル コーポレイション | Patient-worn energy supply device and technology for adjusting its size |
| CN103764222B (en) | 2011-09-01 | 2016-02-10 | 佐尔医药公司 | Wearable monitoring and treatment equipment |
| US9687618B2 (en) | 2011-11-02 | 2017-06-27 | Carefusion 207, Inc. | Ventilation harm index |
| US9177109B2 (en) | 2011-11-02 | 2015-11-03 | Carefusion 207, Inc. | Healthcare facility ventilation management |
| US9821129B2 (en) | 2011-11-02 | 2017-11-21 | Vyaire Medical Capital Llc | Ventilation management system |
| US9072849B2 (en) | 2012-06-29 | 2015-07-07 | Carefusion 207, Inc. | Modifying ventilator operation based on patient orientation |
| US20130110924A1 (en)* | 2011-11-02 | 2013-05-02 | Tom Steinhauer | Wide area ventilation management |
| US9737676B2 (en) | 2011-11-02 | 2017-08-22 | Vyaire Medical Capital Llc | Ventilation system |
| US9058741B2 (en) | 2012-06-29 | 2015-06-16 | Carefusion 207, Inc. | Remotely accessing a ventilator |
| US9352110B2 (en) | 2012-06-29 | 2016-05-31 | Carefusion 207, Inc. | Ventilator suction management |
| EP3610919A1 (en) | 2012-03-02 | 2020-02-19 | Zoll Medical Corporation | A system comprising a wearable therapeutic device |
| JP6655991B2 (en) | 2012-05-30 | 2020-03-04 | レスメッド センサー テクノロジーズ リミテッド | Method and apparatus for monitoring cardiopulmonary health |
| CN104428034A (en) | 2012-05-31 | 2015-03-18 | 佐尔医药公司 | Systems and methods for detecting health disorders |
| CN104870050A (en) | 2012-05-31 | 2015-08-26 | 佐尔医药公司 | Medical monitoring and treatment device with external pacing |
| US10328266B2 (en) | 2012-05-31 | 2019-06-25 | Zoll Medical Corporation | External pacing device with discomfort management |
| US11097107B2 (en) | 2012-05-31 | 2021-08-24 | Zoll Medical Corporation | External pacing device with discomfort management |
| US10525219B2 (en)* | 2012-06-26 | 2020-01-07 | Resmed Sensor Technologies Limited | Methods and apparatus for monitoring and treating respiratory insufficiency |
| US9327090B2 (en) | 2012-06-29 | 2016-05-03 | Carefusion 303, Inc. | Respiratory knowledge portal |
| KR102025571B1 (en)* | 2012-07-27 | 2019-09-27 | 삼성전자주식회사 | Apparatus and method for measuring change in blood pressure caused by breathing control |
| US9999393B2 (en) | 2013-01-29 | 2018-06-19 | Zoll Medical Corporation | Delivery of electrode gel using CPR puck |
| US8880196B2 (en) | 2013-03-04 | 2014-11-04 | Zoll Medical Corporation | Flexible therapy electrode |
| US20140257151A1 (en)* | 2013-03-07 | 2014-09-11 | Hill-Rom Services Pte Ltd. | High frequency chest wall oscillation (hfcwo) data connectivity systems and methods |
| WO2014210510A1 (en) | 2013-06-28 | 2014-12-31 | Zoll Medical Corporation | Systems and methods of delivering therapy using an ambulatory medical device |
| WO2015123198A1 (en) | 2014-02-12 | 2015-08-20 | Zoll Medical Corporation | System and method for adapting alarms in a wearable medical device |
| US9568354B2 (en) | 2014-06-12 | 2017-02-14 | PhysioWave, Inc. | Multifunction scale with large-area display |
| US9943241B2 (en) | 2014-06-12 | 2018-04-17 | PhysioWave, Inc. | Impedance measurement devices, systems, and methods |
| US9949662B2 (en) | 2014-06-12 | 2018-04-24 | PhysioWave, Inc. | Device and method having automatic user recognition and obtaining impedance-measurement signals |
| US9546898B2 (en) | 2014-06-12 | 2017-01-17 | PhysioWave, Inc. | Fitness testing scale |
| US10130273B2 (en) | 2014-06-12 | 2018-11-20 | PhysioWave, Inc. | Device and method having automatic user-responsive and user-specific physiological-meter platform |
| US9498137B2 (en)* | 2014-08-07 | 2016-11-22 | PhysioWave, Inc. | Multi-function fitness scale with display |
| US9693696B2 (en) | 2014-08-07 | 2017-07-04 | PhysioWave, Inc. | System with user-physiological data updates |
| US10201711B2 (en) | 2014-12-18 | 2019-02-12 | Zoll Medical Corporation | Pacing device with acoustic sensor |
| US10136859B2 (en) | 2014-12-23 | 2018-11-27 | Michael Cutaia | System and method for outpatient management of chronic disease |
| US10321877B2 (en) | 2015-03-18 | 2019-06-18 | Zoll Medical Corporation | Medical device with acoustic sensor |
| EP4186548A1 (en) | 2015-04-02 | 2023-05-31 | Hill-Rom Services PTE. LTD. | Mask leakage detection for a respiratory device |
| US10945671B2 (en) | 2015-06-23 | 2021-03-16 | PhysioWave, Inc. | Determining physiological parameters using movement detection |
| US10553306B2 (en) | 2015-11-20 | 2020-02-04 | PhysioWave, Inc. | Scaled-based methods and apparatuses for automatically updating patient profiles |
| US10436630B2 (en) | 2015-11-20 | 2019-10-08 | PhysioWave, Inc. | Scale-based user-physiological data hierarchy service apparatuses and methods |
| US11561126B2 (en) | 2015-11-20 | 2023-01-24 | PhysioWave, Inc. | Scale-based user-physiological heuristic systems |
| US10395055B2 (en) | 2015-11-20 | 2019-08-27 | PhysioWave, Inc. | Scale-based data access control methods and apparatuses |
| US10980483B2 (en) | 2015-11-20 | 2021-04-20 | PhysioWave, Inc. | Remote physiologic parameter determination methods and platform apparatuses |
| US10923217B2 (en) | 2015-11-20 | 2021-02-16 | PhysioWave, Inc. | Condition or treatment assessment methods and platform apparatuses |
| PL3693057T3 (en) | 2015-11-23 | 2023-02-20 | Zoll Medical Corporation | Garments for wearable medical devices |
| US10493224B2 (en) | 2015-12-31 | 2019-12-03 | At&T Intellectual Property I, L.P. | Apparatus and method for improving an artificial respirator |
| US11617538B2 (en) | 2016-03-14 | 2023-04-04 | Zoll Medical Corporation | Proximity based processing systems and methods |
| US10390772B1 (en) | 2016-05-04 | 2019-08-27 | PhysioWave, Inc. | Scale-based on-demand care system |
| US10215619B1 (en) | 2016-09-06 | 2019-02-26 | PhysioWave, Inc. | Scale-based time synchrony |
| US11009870B2 (en) | 2017-06-06 | 2021-05-18 | Zoll Medical Corporation | Vehicle compatible ambulatory defibrillator |
| TWI642025B (en)* | 2017-08-11 | 2018-11-21 | 國立中興大學 | Rapid assessment of moderate to severe sleep breathing |
| JP7234235B2 (en)* | 2017-12-20 | 2023-03-07 | コーニンクレッカ フィリップス エヌ ヴェ | Control unit for use with respiratory assistance devices |
| WO2019178524A1 (en) | 2018-03-16 | 2019-09-19 | Zoll Medical Corporation | Monitoring physiological status based on bio-vibrational and radio frequency data analysis |
| US11568984B2 (en) | 2018-09-28 | 2023-01-31 | Zoll Medical Corporation | Systems and methods for device inventory management and tracking |
| WO2020069308A1 (en) | 2018-09-28 | 2020-04-02 | Zoll Medical Corporation | Adhesively coupled wearable medical device |
| US12001939B2 (en) | 2018-12-11 | 2024-06-04 | Eko.Ai Pte. Ltd. | Artificial intelligence (AI)-based guidance for an ultrasound device to improve capture of echo image views |
| US12322100B2 (en) | 2018-12-11 | 2025-06-03 | Eko.Ai Pte. Ltd. | Automatic clinical workflow that recognizes and analyzes 2D and doppler modality echocardiogram images for automated cardiac measurements and grading of aortic stenosis severity |
| US11931207B2 (en) | 2018-12-11 | 2024-03-19 | Eko.Ai Pte. Ltd. | Artificial intelligence (AI) recognition of echocardiogram images to enhance a mobile ultrasound device |
| US12400762B2 (en) | 2018-12-11 | 2025-08-26 | Eko.Ai Pte. Ltd. | Automatic clinical workflow that recognizes and analyzes 2D and doppler modality echocardiogram images for automated cardiac measurements and diagnosis of cardiac amyloidosis and hypertrophic cardiomyopathy |
| US11446009B2 (en) | 2018-12-11 | 2022-09-20 | Eko.Ai Pte. Ltd. | Clinical workflow to diagnose heart disease based on cardiac biomarker measurements and AI recognition of 2D and doppler modality echocardiogram images |
| EP3902598B1 (en) | 2018-12-28 | 2024-12-04 | ZOLL Medical Corporation | Wearable medical device response mechanisms |
| CN112386224A (en)* | 2019-08-14 | 2021-02-23 | 徐文雄 | Sleep health management system |
| CN112642061A (en) | 2019-10-09 | 2021-04-13 | Zoll医疗公司 | Modular electrotherapy device |
| GB2628495B (en)* | 2019-11-04 | 2024-12-11 | Fisher & Paykel Healthcare Ltd | Breathing assistance apparatuses and/or components thereof and/or uses thereof |
| US12403322B2 (en) | 2021-02-08 | 2025-09-02 | Zoll Medical Corporation | Modular ingress protected electrode system for a wearable defibrillator |
| CN113576434B (en)* | 2021-09-03 | 2024-03-22 | 施丹君 | Ear-hanging human blood oxygen saturation and heart rate monitor |
| AU2022385572A1 (en)* | 2021-11-15 | 2024-05-16 | Fisher & Paykel Healthcare Limited | Data capture, processing, storage and rendering system for breathing assistance apparatus |
Citations (43)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US4944310A (en) | 1981-04-24 | 1990-07-31 | Somed Pty. Ltd. | Device for treating snoring sickness |
| US5105354A (en) | 1989-01-23 | 1992-04-14 | Nippon Kayaku Kabushiki Kaisha | Method and apparatus for correlating respiration and heartbeat variability |
| JPH04161143A (en) | 1990-10-25 | 1992-06-04 | Masahiko Shimizu | Physical exercise recorder |
| US5259373A (en) | 1989-05-19 | 1993-11-09 | Puritan-Bennett Corporation | Inspiratory airway pressure system controlled by the detection and analysis of patient airway sounds |
| US5275159A (en) | 1991-03-22 | 1994-01-04 | Madaus Schwarzer Medizintechnik Gmbh & Co. Kg | Method and apparatus for diagnosis of sleep disorders |
| US5353788A (en) | 1992-09-21 | 1994-10-11 | Miles Laughton E | Cardio-respiratory control and monitoring system for determining CPAP pressure for apnea treatment |
| DE19538473A1 (en) | 1995-10-16 | 1997-04-17 | Map Gmbh | Device and method for the quantitative analysis of sleep disorders |
| US5630413A (en) | 1992-07-06 | 1997-05-20 | Sandia Corporation | Reliable noninvasive measurement of blood gases |
| WO1997028838A1 (en) | 1996-02-12 | 1997-08-14 | New York University | Method and apparatus for optimizing the continuous positive airway pressure for treating obstructive sleep apnea |
| US5704345A (en) | 1993-11-05 | 1998-01-06 | Resmed Limited | Detection of apnea and obstruction of the airway in the respiratory system |
| JPH1094318A (en) | 1996-09-20 | 1998-04-14 | Seirei Ind Co Ltd | Safe device of self-running type thresher |
| US5740795A (en) | 1993-12-03 | 1998-04-21 | Resmed Limited, An Australian Company | Estimation of flow and detection of breathing in CPAP treatment |
| US5769084A (en) | 1996-07-10 | 1998-06-23 | The United States Of America As Represented By The Secretary Of The Navy | Method and apparatus for diagnosing sleep breathing disorders |
| US5794615A (en) | 1994-06-03 | 1998-08-18 | Respironics, Inc. | Method and apparatus for providing proportional positive airway pressure to treat congestive heart failure |
| US5974340A (en) | 1997-04-29 | 1999-10-26 | Cardiac Pacemakers, Inc. | Apparatus and method for monitoring respiratory function in heart failure patients to determine efficacy of therapy |
| US6015388A (en) | 1997-03-17 | 2000-01-18 | Nims, Inc. | Method for analyzing breath waveforms as to their neuromuscular respiratory implications |
| US6152129A (en) | 1996-08-14 | 2000-11-28 | Resmed Limited | Determination of leak and respiratory airflow |
| US6186142B1 (en) | 1997-07-25 | 2001-02-13 | Minnesota Innovative Technologies & Instruments Corporation (Miti) | Control of respiratory oxygen delivery |
| US6237593B1 (en) | 1993-12-03 | 2001-05-29 | Resmed Limited | Estimation of flow and detection of breathing CPAP treatment |
| JP2001513387A (en) | 1997-08-25 | 2001-09-04 | テーマ | A method and apparatus for determining an image of a user's nasal and / or oral respiratory flow. |
| US6332463B1 (en) | 1995-09-15 | 2001-12-25 | Resmed Limited | Flow estimation and compensation of flow-induced pressure swings in CPAP treatment and assisted respiration |
| US6336454B1 (en) | 1997-05-16 | 2002-01-08 | Resmed Limited | Nasal ventilation as a treatment for stroke |
| JP2002505924A (en) | 1998-03-12 | 2002-02-26 | レスピロニクス・インコーポレイテッド | Method and apparatus for supplying positive pressure to the airway of a subject |
| JP2002516159A (en) | 1998-05-22 | 2002-06-04 | レスメッド・リミテッド | Ventilation support for treatment of heart failure and Cheyne-Stokes breathing |
| WO2002047747A1 (en) | 2000-12-11 | 2002-06-20 | Resmed Ltd. | Methods and apparatus for stroke patient treatment |
| US6532957B2 (en) | 1996-09-23 | 2003-03-18 | Resmed Limited | Assisted ventilation to match patient respiratory need |
| US6539940B2 (en) | 1989-09-22 | 2003-04-01 | Respironics, Inc. | Breathing gas delivery method and apparatus |
| WO2003030804A2 (en) | 2001-10-12 | 2003-04-17 | Ric Investments, Inc. | Auto-titration pressure support system and method of using same |
| JP2003516825A (en) | 1999-12-16 | 2003-05-20 | コムピュメディクス スリープ プロプライエタリー リミテッド | Biomask with integrated sensor |
| US6662032B1 (en) | 1999-07-06 | 2003-12-09 | Intercure Ltd. | Interventive-diagnostic device |
| JP2004003813A (en) | 2002-04-14 | 2004-01-08 | Toru Kobayashi | Cooling source |
| US20040003813A1 (en) | 1999-06-30 | 2004-01-08 | Banner Michael J. | Medical ventilator and method of controlling same |
| US20040111040A1 (en) | 2002-12-04 | 2004-06-10 | Quan Ni | Detection of disordered breathing |
| JP2004526470A (en) | 2000-09-25 | 2004-09-02 | レスピロニクス・インコーポレイテッド | Method and apparatus for providing variable positive airway pressure |
| JP2004529797A (en) | 2001-06-15 | 2004-09-30 | ダウ グローバル テクノロジーズ インコーポレイティド | Automotive assembly parts |
| JP2004533483A (en) | 2001-07-03 | 2004-11-04 | アベシア・リミテッド | Process for the preparation of nitrile compounds |
| US20050065567A1 (en) | 2003-09-18 | 2005-03-24 | Cardiac Pacemakers, Inc. | Therapy control based on cardiopulmonary status |
| US6893405B2 (en) | 2002-01-22 | 2005-05-17 | Medcare Flaga Hf | Analysis of Sleep Apnea |
| US20050115561A1 (en) | 2003-08-18 | 2005-06-02 | Stahmann Jeffrey E. | Patient monitoring, diagnosis, and/or therapy systems and methods |
| US6988498B2 (en) | 1997-11-07 | 2006-01-24 | Resmed Limited | Administration of CPAP treatment pressure in presence of apnea |
| US20060060198A1 (en) | 2004-09-17 | 2006-03-23 | Acoba, Llc | Method and system of scoring sleep disordered breathing |
| WO2007101297A1 (en) | 2006-03-06 | 2007-09-13 | Resmed Ltd | Determination of apnea/hypopnea during cpap treatment |
| US20070250345A1 (en)* | 2006-04-24 | 2007-10-25 | James Walker | Electronic medical record system, method, and computer process for the testing, diagnosis, and treatment of sleep disorders |
- 2005
- 2005-03-30USUS10/598,914patent/US7878198B2/ennot_activeExpired - Fee Related
- 2010
- 2010-12-30USUS12/982,536patent/US8517014B2/ennot_activeExpired - Lifetime
- 2013
- 2013-08-15USUS13/967,517patent/US10610167B2/ennot_activeExpired - Fee Related
Patent Citations (50)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US4944310A (en) | 1981-04-24 | 1990-07-31 | Somed Pty. Ltd. | Device for treating snoring sickness |
| US5105354A (en) | 1989-01-23 | 1992-04-14 | Nippon Kayaku Kabushiki Kaisha | Method and apparatus for correlating respiration and heartbeat variability |
| US5259373A (en) | 1989-05-19 | 1993-11-09 | Puritan-Bennett Corporation | Inspiratory airway pressure system controlled by the detection and analysis of patient airway sounds |
| US6539940B2 (en) | 1989-09-22 | 2003-04-01 | Respironics, Inc. | Breathing gas delivery method and apparatus |
| JPH04161143A (en) | 1990-10-25 | 1992-06-04 | Masahiko Shimizu | Physical exercise recorder |
| US5275159A (en) | 1991-03-22 | 1994-01-04 | Madaus Schwarzer Medizintechnik Gmbh & Co. Kg | Method and apparatus for diagnosis of sleep disorders |
| US5630413A (en) | 1992-07-06 | 1997-05-20 | Sandia Corporation | Reliable noninvasive measurement of blood gases |
| US5353788A (en) | 1992-09-21 | 1994-10-11 | Miles Laughton E | Cardio-respiratory control and monitoring system for determining CPAP pressure for apnea treatment |
| EP1488743A2 (en) | 1993-11-05 | 2004-12-22 | Resmed Limited | Control of CPAP Treatment |
| US5704345A (en) | 1993-11-05 | 1998-01-06 | Resmed Limited | Detection of apnea and obstruction of the airway in the respiratory system |
| US5740795A (en) | 1993-12-03 | 1998-04-21 | Resmed Limited, An Australian Company | Estimation of flow and detection of breathing in CPAP treatment |
| US6237593B1 (en) | 1993-12-03 | 2001-05-29 | Resmed Limited | Estimation of flow and detection of breathing CPAP treatment |
| US5794615A (en) | 1994-06-03 | 1998-08-18 | Respironics, Inc. | Method and apparatus for providing proportional positive airway pressure to treat congestive heart failure |
| US6332463B1 (en) | 1995-09-15 | 2001-12-25 | Resmed Limited | Flow estimation and compensation of flow-induced pressure swings in CPAP treatment and assisted respiration |
| DE19538473A1 (en) | 1995-10-16 | 1997-04-17 | Map Gmbh | Device and method for the quantitative analysis of sleep disorders |
| WO1997028838A1 (en) | 1996-02-12 | 1997-08-14 | New York University | Method and apparatus for optimizing the continuous positive airway pressure for treating obstructive sleep apnea |
| JP2000504602A (en) | 1996-02-12 | 2000-04-18 | ニューヨーク ユニヴァーシティー | Method and apparatus for optimizing continuous positive airway pressure to treat obstructive sleep apnea |
| US5769084A (en) | 1996-07-10 | 1998-06-23 | The United States Of America As Represented By The Secretary Of The Navy | Method and apparatus for diagnosing sleep breathing disorders |
| US6152129A (en) | 1996-08-14 | 2000-11-28 | Resmed Limited | Determination of leak and respiratory airflow |
| JPH1094318A (en) | 1996-09-20 | 1998-04-14 | Seirei Ind Co Ltd | Safe device of self-running type thresher |
| US6532957B2 (en) | 1996-09-23 | 2003-03-18 | Resmed Limited | Assisted ventilation to match patient respiratory need |
| US6015388A (en) | 1997-03-17 | 2000-01-18 | Nims, Inc. | Method for analyzing breath waveforms as to their neuromuscular respiratory implications |
| US5974340A (en) | 1997-04-29 | 1999-10-26 | Cardiac Pacemakers, Inc. | Apparatus and method for monitoring respiratory function in heart failure patients to determine efficacy of therapy |
| US6336454B1 (en) | 1997-05-16 | 2002-01-08 | Resmed Limited | Nasal ventilation as a treatment for stroke |
| US6186142B1 (en) | 1997-07-25 | 2001-02-13 | Minnesota Innovative Technologies & Instruments Corporation (Miti) | Control of respiratory oxygen delivery |
| JP2001513387A (en) | 1997-08-25 | 2001-09-04 | テーマ | A method and apparatus for determining an image of a user's nasal and / or oral respiratory flow. |
| US6988498B2 (en) | 1997-11-07 | 2006-01-24 | Resmed Limited | Administration of CPAP treatment pressure in presence of apnea |
| JP2002505924A (en) | 1998-03-12 | 2002-02-26 | レスピロニクス・インコーポレイテッド | Method and apparatus for supplying positive pressure to the airway of a subject |
| JP2002516159A (en) | 1998-05-22 | 2002-06-04 | レスメッド・リミテッド | Ventilation support for treatment of heart failure and Cheyne-Stokes breathing |
| US6532959B1 (en) | 1998-05-22 | 2003-03-18 | Resmed, Ltd. | Ventilatory assistance for treatment of cardiac failure and cheyne-stokes breathing |
| US20040003813A1 (en) | 1999-06-30 | 2004-01-08 | Banner Michael J. | Medical ventilator and method of controlling same |
| US6662032B1 (en) | 1999-07-06 | 2003-12-09 | Intercure Ltd. | Interventive-diagnostic device |
| JP2003516825A (en) | 1999-12-16 | 2003-05-20 | コムピュメディクス スリープ プロプライエタリー リミテッド | Biomask with integrated sensor |
| JP2004526470A (en) | 2000-09-25 | 2004-09-02 | レスピロニクス・インコーポレイテッド | Method and apparatus for providing variable positive airway pressure |
| WO2002047747A1 (en) | 2000-12-11 | 2002-06-20 | Resmed Ltd. | Methods and apparatus for stroke patient treatment |
| US20020185130A1 (en)* | 2000-12-11 | 2002-12-12 | Wright Jonathan Caldwell | Methods and apparatus for stroke patient treatment |
| US6832609B2 (en) | 2000-12-11 | 2004-12-21 | Resmed Limited | Methods and apparatus for stroke patient treatment |
| JP2004522483A (en) | 2000-12-11 | 2004-07-29 | レスメッド・リミテッド | Method and apparatus for treating a stroke patient |
| JP2004529797A (en) | 2001-06-15 | 2004-09-30 | ダウ グローバル テクノロジーズ インコーポレイティド | Automotive assembly parts |
| JP2004533483A (en) | 2001-07-03 | 2004-11-04 | アベシア・リミテッド | Process for the preparation of nitrile compounds |
| WO2003030804A2 (en) | 2001-10-12 | 2003-04-17 | Ric Investments, Inc. | Auto-titration pressure support system and method of using same |
| US6893405B2 (en) | 2002-01-22 | 2005-05-17 | Medcare Flaga Hf | Analysis of Sleep Apnea |
| JP2004003813A (en) | 2002-04-14 | 2004-01-08 | Toru Kobayashi | Cooling source |
| WO2004049930A2 (en) | 2002-12-04 | 2004-06-17 | Cardiac Pacemakers, Inc. | Detection of disordered breathing |
| US20040111040A1 (en) | 2002-12-04 | 2004-06-10 | Quan Ni | Detection of disordered breathing |
| US20050115561A1 (en) | 2003-08-18 | 2005-06-02 | Stahmann Jeffrey E. | Patient monitoring, diagnosis, and/or therapy systems and methods |
| US20050065567A1 (en) | 2003-09-18 | 2005-03-24 | Cardiac Pacemakers, Inc. | Therapy control based on cardiopulmonary status |
| US20060060198A1 (en) | 2004-09-17 | 2006-03-23 | Acoba, Llc | Method and system of scoring sleep disordered breathing |
| WO2007101297A1 (en) | 2006-03-06 | 2007-09-13 | Resmed Ltd | Determination of apnea/hypopnea during cpap treatment |
| US20070250345A1 (en)* | 2006-04-24 | 2007-10-25 | James Walker | Electronic medical record system, method, and computer process for the testing, diagnosis, and treatment of sleep disorders |
Non-Patent Citations (8)
| Title |
|---|
| Clark, et al., Assessment of Inspiratory Flow Limitation Invasively and Noninvasively during Sleep, Am J. Respir. Crit. Care Med, vol. 158, pp. 713-722, 1998. |
| European Patent Office; Supplementary Search Report, corresponding patent application No. 05734977.1; dated Jul. 23, 2009. |
| Frey et al ., J. Applied Physiology, 91; 1687-1693 (2001). |
| International Search Report for Application No. PCT/AU2008/000647 dated Aug. 13, 2008. |
| Japanese Office Action for Application No. P2011-035025 dated Sep. 4, 2012. |
| Japanese Patent Office; Notice of Reasons for Rejection; corresponding to patent application No. P2007-506506; dated Oct. 26, 2010. |
| Kirkness et al., Prog Respir Res. 35; 79-89 (2006). |
| Marcus et al., J Applied PhysioLogy, 87; 1448-1454 (1999). |
Cited By (2)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| USD1014517S1 (en) | 2021-05-05 | 2024-02-13 | Fisher & Paykel Healthcare Limited | Display screen or portion thereof with graphical user interface |
| US20230104018A1 (en)* | 2021-10-05 | 2023-04-06 | Ndustry-Academic Cooperation Foundation, Yonsei University | Cardiovascular disease risk analysis system and method considering sleep apnea factors |
Also Published As
| Publication number | Publication date |
|---|---|
| US20110139155A1 (en) | 2011-06-16 |
| US7878198B2 (en) | 2011-02-01 |
| US20070161913A1 (en) | 2007-07-12 |
| US20130331713A1 (en) | 2013-12-12 |
| US8517014B2 (en) | 2013-08-27 |
Similar Documents
| Publication | Publication Date | Title |
|---|---|---|
| US10610167B2 (en) | Methods and apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing | |
| EP1729841B1 (en) | Apparatus for monitoring the cardiovascular condition of patients with sleep disordered breathing | |
| US6832609B2 (en) | Methods and apparatus for stroke patient treatment | |
| US10856802B2 (en) | Methods and apparatus for heart failure treatment | |
| EP2147693B1 (en) | Apparatus for detecting and treating heart failure | |
| CN115052648B (en) | Method and apparatus for determining and/or predicting sleep and respiratory behavior that governs airway pressure | |
| AU2002220369A1 (en) | Methods and apparatus for stroke patient treatment | |
| AU2007201865B2 (en) | Methods and Apparatus for Stroke Patient Treatment |
Legal Events
| Date | Code | Title | Description |
|---|---|---|---|
| STCV | Information on status: appeal procedure | Free format text:ON APPEAL -- AWAITING DECISION BY THE BOARD OF APPEALS | |
| AS | Assignment | Owner name:RESMED PTY LTD, AUSTRALIA Free format text:CHANGE OF NAME;ASSIGNOR:RESMED LIMITED;REEL/FRAME:049454/0442 Effective date:20181206 | |
| STCV | Information on status: appeal procedure | Free format text:BOARD OF APPEALS DECISION RENDERED | |
| STPP | Information on status: patent application and granting procedure in general | Free format text:DOCKETED NEW CASE - READY FOR EXAMINATION | |
| STPP | Information on status: patent application and granting procedure in general | Free format text:NOTICE OF ALLOWANCE MAILED -- APPLICATION RECEIVED IN OFFICE OF PUBLICATIONS | |
| ZAAA | Notice of allowance and fees due | Free format text:ORIGINAL CODE: NOA | |
| ZAAB | Notice of allowance mailed | Free format text:ORIGINAL CODE: MN/=. | |
| AS | Assignment | Owner name:RESMED CORP., CALIFORNIA Free format text:ASSIGNMENT OF ASSIGNORS INTEREST;ASSIGNORS:FARRELL, MICHAEL;HEBBLEWHITE, MALCOLM RONALD;STEWART, DEIRDRE;AND OTHERS;SIGNING DATES FROM 20120312 TO 20121024;REEL/FRAME:051922/0060 Owner name:RESMED LIMITED, AUSTRALIA Free format text:ASSIGNMENT OF ASSIGNORS INTEREST;ASSIGNOR:RESMED CORP.;REEL/FRAME:051922/0496 Effective date:20130729 Owner name:RESMED CORP., CALIFORNIA Free format text:STATEMENT OF OWNERSHIP;ASSIGNOR:RANDOLPH, ROBIN;REEL/FRAME:052885/0885 Effective date:20130104 | |
| STPP | Information on status: patent application and granting procedure in general | Free format text:PUBLICATIONS -- ISSUE FEE PAYMENT VERIFIED | |
| STCF | Information on status: patent grant | Free format text:PATENTED CASE | |
| FEPP | Fee payment procedure | Free format text:MAINTENANCE FEE REMINDER MAILED (ORIGINAL EVENT CODE: REM.); ENTITY STATUS OF PATENT OWNER: LARGE ENTITY | |
| LAPS | Lapse for failure to pay maintenance fees | Free format text:PATENT EXPIRED FOR FAILURE TO PAY MAINTENANCE FEES (ORIGINAL EVENT CODE: EXP.); ENTITY STATUS OF PATENT OWNER: LARGE ENTITY | |
| STCH | Information on status: patent discontinuation | Free format text:PATENT EXPIRED DUE TO NONPAYMENT OF MAINTENANCE FEES UNDER 37 CFR 1.362 | |
| FP | Lapsed due to failure to pay maintenance fee | Effective date:20240407 |